Article content
Scott Williams credits Canada’s only stroke ambulance for saving his life last summer.
advertisement 2
Article content
The Rich Valley, Alta., cattle rancher began to feel unwell on Aug. 5, 2021, while checking the quality of his hay. At one point he stumbled, and at first, he thought he might have had one too many cups of coffee.
His wife drove him back to the house, and when he went to lay down in bed, he realized something was wrong. He told his wife he needed to get to a hospital. By the time he made it out the front door, Williams said his left leg was “exceptionally weak.”
“Two miles down the road, I told her that I’m pretty sure I’m having a stroke because by now I couldn’t feel my left leg, my left arm and I noticed that my speech was starting to slur and I started to atrophy which meant my head was kicked over to the left side,” he said, crediting his background in emergency services with identifying the symptoms of a stroke.
advertisement 3
Article content
Rich Valley is about 88 kilometers northwest of Edmonton and when they reached the Barrhead Hospital, about 120 kilometers northwest of the capital, they were told it was not a hospital equipped to treat strokes and a doctor contacted the stroke ambulance.
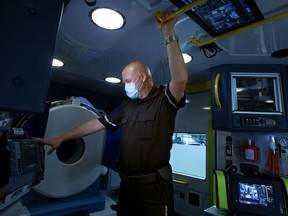
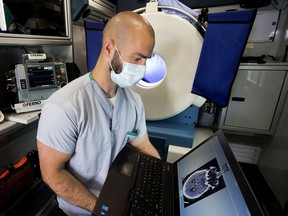
The ambulance is the only one of its kind in Canada and has been operating as a pilot project since 2017, funded by the University Hospital Foundation. It contains a CT scan, which does imaging in about 70 seconds, and sends about 100 images back to the University of Alberta Hospital.
The ambulance, running Monday to Friday, 8 am to 4 pm, has a crew of five: an advanced care paramedic, a primary care paramedic, a specially trained nurse, a CT technologist to run the scanner, and a stroke fellow who’s a neurologist training in stroke. The team will contact a neurologist back at the hospital and discuss the images.
advertisement 4
Article content
“We’ll come up with a treatment plan whether that’s to give the patient to thrombolytic, so the clot-buster, or to transport them back where they came from because we’re not finding a stroke,” said primary care paramedic Kelly Brown .
It has a 250-kilometre catchment area from the U of A, in any direction, and will normally meet up with another paramedic crew. On the day of Williams’ stroke, the Barrhead paramedic crew transported him and met the stroke ambulance at the Onoway High School, where they proceeded to do their treatment.
“By the time we brought it to the outskirts of Edmonton, I had already started to get movement back in my toes and my fingers,” Willams said. “By the time we got to the U of A hospital, I even had more movement from the knee down and my arm from the elbow to my fingers.”
advertisement 5
Article content
At the hospital, Williams underwent further testing.
“Within maybe eight hours, they came and told me that it was a miracle that I was alive and I was doing remarkably well,” he said.
Only in the last 30 years or so have advancements been made in stroke treatment, said Dr. Tom Jeerakathil, a stroke neurologist. The stroke ambulance is one of those innovations.
“On the average, we treat rural patients about 68 minutes faster than standard care, which translates into about 136,000 brain cells saved,” he said, noting the average loss is about two million cells a minute.
“On the average, we’re treating urban patients about 37 minutes faster. Now, that doesn’t seem like a lot, but on the average, we’re treating urban patients in the golden hour after stroke onset, within an hour of onset of symptoms, which is quite uncommon in other systems, unless they’ve got stroke ambulances.”
Williams, who was 56 at the time of his stroke, was released from the hospital within a few days. The only lingering effect he deals with is fatigue.
“I’d hate to think what would have happened if that stroke ambulance hadn’t been on duty, or if it had been busy,” he said. “I think I would have been bugged.”